PRIME
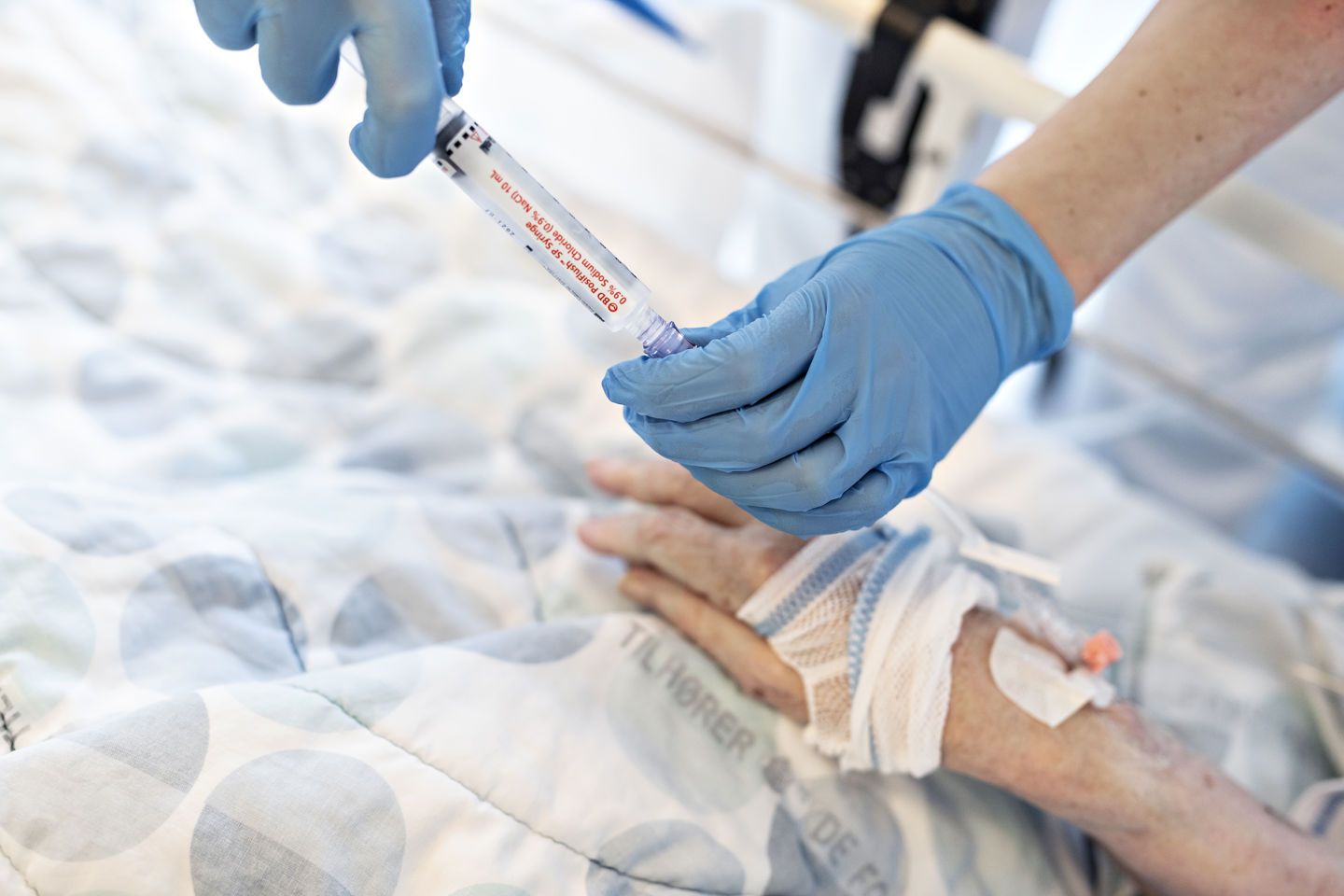
Personalized medicine raises pressing questions about priority setting. How to draw the line?
The categorization of disease is a pillar not only for medical reasoning, but also for the distribution of healthcare resources and patients’ access to care.
While disease categories may seem to neutrally reflect biological differences, social studies of science and medicine demonstrate that conceptions of disease and its proper treatment are also shaped by cultural beliefs, social processes and political interests. Yet it is not well understood how the categorization of disease influences and is influenced by economic concerns.
The current surge of personalized medicine makes the question of which categories of human differences and similarities should influence economic prioritizations all the more pressing.
Personalized medicine refers to ambitions of redefining diagnostic categories and targeting therapies to genetic markers of disease, leading to more granular patient groups. A touted promise of personalized medicine is to reduce overtreatment and overspending through greater accuracy. However, personalized therapies also bring new uncertainties and unprecedentedly high pricing. Often, it is uncertain how genetic traits relate to phenotypic characteristics. Moreover, small patient populations challenge established scientific methods for determining cost-effectiveness, though the rising prices make prioritization more pressing.
Project aims
Based on ethnographic fieldwork in four clinical settings, we investigate how disease categorization and economic concerns influence each other when treatments become increasingly personalized. We also examine the implications of this interplay for patients’ access to treatment and their experiences of community and marginalization in the Danish welfare state.
Research questions guiding the project:
- Which ideas about human similarities and differences are enacted when treatment decisions that involve personalized medicine are made?
- How do economic concerns and government techniques influence the categorization of disease and patients’ access to treatment?
- Which implications can the interplay between disease categorization and economic concerns have for patients’ experiences of community and marginalization in the Danish welfare state?
Our aim is to provide insights that can establish a basis for public dialogue about the economic, social and ethical implications of medical innovation. The processes of priority setting that arise along with medical innovation are not merely technocratic process – they contribute to establishing ideas about what constitutes a valuable treatment for whom. We seek to develop concepts that can capture and foster debate about these issues.

Universal Access, Differentiate Care is an interdisciplinary research project that investigates the interplay between economic concerns and disease categorization amidst the current surge of ’personalized medicine’ in Denmark.
Subprojects
This subproject investigates how economic concerns shape treatment access for children with the rare disease 5q Spinal Muscular Atrophy (5q SMA). While the genetic basis for 5q SMA has been known for a long time, there was no active treatment until 2017 when the first therapy was marketed. The therapy is targeted the genetic deficiency that causes the loss of muscle power.
The new treatment became the center of a public controversy as it entered the Danish healthcare system because only some patients could access the treatment. Based on cost-effectiveness calculations, national guidelines restrict the use of the therapy to the most severely affected children. Since then, new therapies have been marketed and new lines drawn that shape the treatment possibilities of the SMA population.
This subproject will explore how the boundaries for treatment access are established, negotiated and handled in clinical practice, and what these processes of boundary drawing imply for SMA families’ experiences of community with other patients and the Danish welfare state.
This subproject investigates the introduction of gene therapy in the treatment of adolescents with rare eye diseases such as Lebers congental amaurosis with mutations in the RPE65-gene (LCA2). LCA2 is a slowly progressing illness that eventually leads to blindness.
Because of the high costs and uncertain long-term effects of the therapy, Danish Medicines Council excluded the treatment from publicly funded healthcare services. However, in 2020, access was established after a new type of payment agreement was made between the manufacturer and the Danish authorities. Thus, the gene therapy represents not only a medical, but also an economic, breakthrough. For the first time in Denmark an agreement has been made, which implies that the public has to pay for only those patients who have sufficient benefit of the medicine. But how does one determine the difference between sufficient and insufficient benefit or value of the therapy?
This subproject explores which notions of treatment value are made visible/invisible when regulators, manufacturers, clinicians, patients and relatives negotiate access to the therapies.
In collaboration with the research project TRANSLATE [indsæt link], this subproject investigates experimental attempts at re-diagnosing patients with diabetes. The ambition of re-diagnosis is to use genetic markers to identify the about 2% of the diabetes population who has a rare, congenital type of diabetes, which do not fit the widespread distinction between type 1 and type 2 diabetes. For these patients, the identification of the genetic basis of their condition may contribute to alleviate the risk of stigma usually associated with type 2 diabetes as a ‘life style disease’. Moreover, in contrast to other forms of diabetes, these patients do not need insulin to manage their condition. As chronic treatment may be terminated, cost savings can be expected for the publicly funded healthcare system.
The subproject explores how ambitions of reducing overtreatment and overspending through genetic re-diagnosing interact with patients’ identities and notions of ‘good’ chronic care as their disease category is transformed.
The catalogue of therapies available for incurable lung cancer is rapidly expanding. If one treatment ceases to work, another one is often available. As the number of treatment options increases, the border between active treatment and being dying becomes a matter of (re-)negotiation: When have patients had enough life-prolonging treatment and what concerns about costs, care and of a good death are involved in such considerations?
This sub project explores how the limit separating the continuation of treatment and the beginning of dying is defined, negotiated and handled in the oncology clinic. The project examines interactions between oncologists, patients, relatives and other professionals, and the practical circumstances and alternative trajectories available, as the transition between life-prolonging treatment and palliative care is settled.

Project organization
The project is led by senior researcher and PI Sarah Wadmann.
The project team includes: researcher Amalie Martinus Hauge, senior researcher Laura Emdal Navne, and ph.d. student Anna Brueckner Johansen.
The international advisory board of the project includes:
- Prof. Mette Nordahl Svendsen, University of Copenhagen
- Prof. Stefan Timmermans, University of California, LA
- Prof. Barbara Prainsack, Vienna University
- Prof. Tiago Moreira, Durham University
- Prof. Susi Geiger, University College Dublin
- Prof. Vololona Rabeharisoa, CSI-Mines ParisTech
The project group also collaborates with the research project TRANSLATE led by Prof. Torben Hansen, University of Copenhagen, and the research project MeInWe led by Prof. Mette Nordahl Svendsen, University of Copenhagen [indsæt link til projektet]
Dissemination
-
Navne, L.E., Wadmann, S., Olesen, I., Hansen, T., Thuesen, A.C.B. & Svendsen, M.N. 2025. Whole Genome, Part Population: Protection, Representation and Postcolonial Politics in Precision medicine. Social Science & Medicine, https://doi.org/10.1016/j.socscimed.2025.117998
-
Hauge, A.M. & Andersen, D.B. 2025. Who cares about the dying? – Unpacking integration of palliative care and oncology in the Danish context. Health Sociology Review, 34(1):59-76. https://doi.org/10.1080/14461242.2025.2467908
-
Johansen, A.B. & Navne, L.E. 2024. “The Best I Could”: Future Orientations for Danish Women with Gestational Diabetes. Medical Anthropology, 43(6):509-521. https://doi.org/10.1080/01459740.2024.2384726
-
Johansen, A.B., Geiger, S. & Wadmann, S. 2025. Temporal Layering: How Past, Future and Present Intersect in the Valuation of Pharmaceutical Innovation. Valuation Studies, 12(1):143-170. https://doi.org/10.3384/VS.2001-5992.2025.12.1.143-170.
-
Wadmann, S., Sørensen, M.S. & Højgaard, B. 2024. Health technology assessments of new specialized therapies: A typology of key challenges and potential policy solutions. Health Policy and Technology, 13(3):100890. https://doi.org/10.1016/j.hlpt.2024.100890
-
Wadmann, S., Johansen, A.B., Born, A.P. & Kessel, L. 2024. Infrastructuring precision medicine: Making gene therapies for rare diseases workable in practice, Social Science & Medicine, 351:116966. https://doi.org/10.1016/j.socscimed.2024.116966
-
Wadmann, S. 2023. Disease Classification: A Framework for Analysis. SSM – Qualitative Research in Health, 3:100217, https://doi.org/10.1016/j.ssmqr.2023.100217
-
Wadmann, S., Hauge, A.M. & Navne, L.E. 2023. Good conduct in a context of rationing. A case study of how frontline professionals deal with distributive dilemmas of novel gene therapies, Sociology of Health & Illness, https://doi.org/10.1111/1467-9566.13608
-
Hauge, A.M. 2023. "Regulating diagnosis—Molecular and regulatory sub‐stratifications of lung cancer treatment." Sociology of Health & Illness, https://onlinelibrary.wiley.com/doi/full/10.1111/1467-9566.13693
-
Wadmann, S. 2025. Priority setting and patient rights: Co-production of medical and regulatory innovation in the Danish welfare state. BCEPS International Symposium, Bergen, 18.6.2025
-
Svendsen, M.N. & Navne, L.E. 2025. Genomes as doppelgangers in transnational relations, Nordic STS conference, Stockholm, 11.6.2025
-
Johansen, A.B. 2025. Curation of value from flesh to fact: Visual experience and the objective test result. Nordic STS conference, Stockholm, 11.6.2025
-
Navne, L.E. & Tuesen, A.C.B. 2025. Making a rare diabetes population: Protection, representation and postcolonial politics in precision medicine, Gravity Seminar, for CBMR Center for Metabolic Research, Copenhagen, 28.5.2025
-
Johansen, A.B. 2025. Curation of value from flesh to fact: Visual experience and the objective test result. Oslo University, Oslo, 26.3.2025
-
Wadmann, S. 2024. Samproduktion af medicinsk og regulatorisk innovation i Danmark. Norsk Helsetjenesteforskningskonference Bergen, 13.11.2024
-
Navne, L.E. 2024. Genomic Medicine in Greenland: Ethical implications of introducing Precision Medicine in Greenland. Grønlandsmøde i Novo Nordisk Metabolismecenter, København, 04.03.2024
-
Navne, L.E. 2024 Patienters erfaringer med MODY: Brug af genetiske tests i diabetesudredning. Obstetrisk temadag, Rigshospitalet, 03.04.2024
-
Wadmann, S. 2024. Drawing the line: Principles of priority setting and the legacy of Spinraza, workshop: Etiske hensyn i dansk sundhedsprioritering, København, 12.1.2024.
-
Hauge, A.M. 2023. Prioritering af ny medicin på kræftområdet. Kræftens Bekæmpelse, København, 29. August 2023.
- Johansen, A.B. 2023. Individualized treatment and bureaucratic impartiality: the paradox of fairness. Encounters at the limits of the Welfare State, MEGA seminar, Sønderborg, 21-23 August 2023.
- Spalletta, O., Heinsen, L.L. and Johansen, A.B. 2023. Ordinary Suffering. Encounters at the limits of the Welfare State, MEGA seminar, Sønderborg, 21-23 August 2023.
- Johansen, A.B., 2023. “I would at least think that I have done the best I could” – future orientation through genetic testing. Desirable/Undesirable Futures: Scholarship on the Political, Ethical, and Moral Economies of Post-Pandemic Recovery, Vancouver, 11-13 July 2023
- Hauge, A.M. 2023. Regulating diagnosis– Molecular and regulatory sub-stratifications of lung cancer treatment. NOSTS, Oslo, 7-9 June 2023.
- Johansen, A.B., Geiger, S. and Wadmann, S. 2023. Valuing pharmaceutical innovation: Temporal layering in the biography of a gene therapy. Medical innovation: tracking transformations in the production, governance, clinical practice and access to medicines, Nordic STS, Oslo, 7-9 June 2023.
- Navne, L.E., Wadmann, S. and Svendsen, M.N. 2023. Whole Genome, Part Population:
Clinicians’ Ethical Concerns in Recruiting Diabetes Patients for Whole Genome Sequencing. Nordic STS, Oslo, 7-9 June 2023. - Wadmann, S., Johansen, A.B., Born, A.P. and Kessel, L. 2023. Infrastructuring precision medicine: Making gene therapies for rare diseases workable in clinical practice. Nordic STS, Oslo, 7-9 June 2023.
- Wadmann, S., Navne, L.E., Hauge, A.M., Johansen, A.B. and Martin, P. 2023. Conference panel: Medical innovation: tracking transformations in the production, governance, clinical practice and access to medicines. Nordic STS, Oslo, 7-9 June 2023.
- Johansen, A.B., Geiger, S. and Wadmann, S. 2023. “Good critique” at the intersection between the anthropology of value and pragmatist valuation studies. Workshop on The Good Economy, Paris, 12-13 January 2023.
- Navne, L.E. 2022. Patienterfaringer med MODY. Temadag om MODY på Steno Diabetes Center, København, 7. December 2022.
- Wadmann, S. 2022. How to draw the line? Economic prospects and priority setting in precision medicine. Seminar, Nationalt Genomcenter, 17. November 2022.
- Wadmann, S. 2022. Personlig medicin – hvilke prioriteringsdilemmaer opstår? Vov at Vide – Danmarks Frie Forskningsfonds og Folkeuniversitetets festforelæsninger, Odense, 27. oktober 2022
- Wadmann, S. 2022. Personlig medicin – hvilke prioriteringsdilemmaer opstår? Vov at Vide – Danmarks Frie Forskningsfonds og Folkeuniversitetets festforelæsninger, København, 1. november 2022
- Navne, L.E. ”It’s a strange name and it doesn’t mean anything”: Patient and family experiences of new disease labels in genomic medicine, ICPerMed Conference, Paris 5-6 October 2022.
- Navne, L.E. Fagpersoner og patienters forventninger til og erfaringer med exom- og helgenomsekventering. Klinisk genetisk afdeling, Århus Universitetshospital, 12. September 2022.
- Hauge, A.M. Diagnostic layers or allocative categories? The Case of Precision Medicine for Lung Cancer. Organizational Behaviour in Health, Birmingham, 10-13 September 2022.
- Wadmann, S., Navne, L.E. & Hauge, M. Cooling the patient out: Distributed decision-making and heated debates over access to advanced therapies, EASST, 3-6 July 2022, Madrid.
- Wadmann, S., Navne, L.E., Hauge, M. & Martin, P. Conference Panel: Pharmaceutical transformations: Advanced therapies, personalized medicine and the remaking of healthcare? EASST 3-6 July 2022, Madrid.
- Johansen, A.B. & Navne, L.E. Lost in translation? Personalized medicine as a sociotechnical imaginary. Genomic Justice and the Ethics of Data workshop, Trondheim, 15-17 June 2022.
- Wadmann, S. 2022. Lighed og forskel: Prioritering og personlig medicin i den danske velfærdsstat. Videnskabernes Selskab, 4 April 2022.
- Medicin: Nye avancerede terapier har haft en langsom start, men har potentiale til at stikke af. Videnskab.dk d. 5. januar 2025
-
Forskere advarer mod urealistiske forventninger til personlig medicin. Altinget Sundhed, 13.12.2023,
-
Sundhedsrevolution? I fremtiden kan du måske sende dine organer til syn. Videnskab.dk, 11.9.2022.
- Interview til tema-nummer om personlig medicin, Med. Nr. 20 s. 20-23. Lægemiddelindustriforeningen (lif), marts 2022.
-
Laura Emdal Navne was awarded a travelling grant from the Carlsberg Foundation in 2023 to undertake a research stay in Greenland and develop scientific collaborations. https://www.carlsbergfondet.dk/det-har-vi-stoettet/cf23-1507/
-
Amalie Martinus Hauge was awarded the Inge Lehmann and the Sapere Aude Research Grant from the Independent Research Fund Denmark in 2024 to undertake the research project entitled: “Working at the Boundaries of Dying: Dying Trajectories, Medical Futility and Transition Work in the 21st century”. https://dff.dk/en/our-funded-projects/meet-the-researchers/research-leaders/eksterne-personer-en/research-leaders-2024/amalie-martinus-hauge/
- Anna Brueckner Johansen’s article “‘The best I could’: Future Orientations for Danish Women with Gestational Diabetes” was awarded the annual CAR Student Paper Prize 2024 by the Council on Anthropology and Reproduction. The article is published together with Laura Emdal Navne and can be downloaded here: https://doi.org/10.1080/01459740.2024.2384726
- Amalie Hauge’s conference paper ’Diagnostic layers or allocative categories? The Case of Precision Medicine for Lung Cancer’ was awarded the ‘highly commended early carreer’ price at the Organizational Behaviour in Health conference 2022.
